Anatomy of the Eye for Medical Students: Let’s start with Opthalmology with its basic Anatomy of the Eye. I made this blog useful mainly for undergraduate medical students and those who are preparing for NExT, PLAB, and USMLE exams.
First, there will be clear-cut exam-oriented points on Anatomy of the Eye notes for Medical Students then at the bottom there will be a link to the Free online MCQs on Anatomy of the Eye and these MCQs are specially made up for NExT, PLAB, and USMLE exams. Jump to,
Page Contents
ToggleAnatomy of the Eye for Medical Students
- 6 ml volume
- Suspended in an orbit of 30 ml
- Encapsulated by Tenon’s capsule and fat cushion
- Supported by Lockwood’s ligament from the orbit like a hammock
- Accessory eyeball structures – Extraocular muscles, fat, eyebrows, lacrimal gland
- 3 layers – Outer fibrous, Middle vascular, and inner neural layer
Outer fibrous layer
- 3 parts – Cornea, Sclera, and Limbus
- Cornea – Upper eyelids rest 2 mm below the sclera
- Anterior 1/6th of the outer fibrous layer is made up of the cornea
- Posterior 5/6th of the outer fibrous layer is made up of the sclera
- Sclera -maintains the shape and attachment of Extraocular muscles
- Extraocular muscles – 4 recti (Superior, Inferior, Lateral and Medial) and 2 obliques (Superior and Inferior)
- The thinnest part of Sclera – Just behind the attachment of recti muscles (Carefully handled in Squint surgeries)
- Thickest in the posterior pole
- 3 layers of the sclera – Episclera, Stroma and Lamina fusca
- White in color and icteric in Jaundice
- Cornea – 11.5 mm – Prolate spheroid in shape – More curved in the center
- Keratometer and Placido’s Disc used to measure the curvature of the cornea
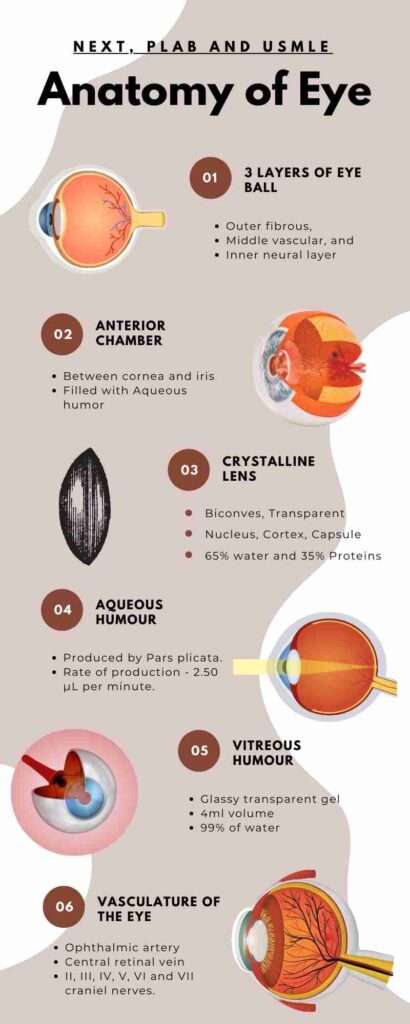
- Highly transparent (90%) light transmission – The regular stromal arrangement and the Na K ATPase pump made the cornea so much transparent.
- 6 layers of the cornea – Epithelium, Bowman’s membrane(Corneal scares), Stroma (90% of the thickness of the cornea), Dua’s layer, Descemet’s membrane, and the Endothelium (Single layer of hexagonal cells)
- The thinnest part is the center (500 to 600μ) and the thickest part is the periphery.
- IOP depends on the Central Corneal Thickness (CCT)
- Pachymeter is used to determine the thickness of the cornea.
- The most powerful refracting surface of the eye – 43D (70% of the total power of the eye)
- Avascular – Glucose from AH and Oxygen from the air, tear film, and AH
- Sensory nerve supply – Ophthalmic branch of the fifth cranial nerve
- 3 parts of Ophthalmic branch – Nasociliary, Lacrimal and Frontal
- Limbus – Junction between the cornea and sclera
- Surgical limbus 2 mm zone
- Corneal stem cells at limbus – palisades of Vogt
- Limbal stem cell deficiency – Regenerative capacity decreases
- Mainly due to Chemical injury, prolonged use of contact lenses, Pterygium,…
- Signs of LSCD – Cells breakdown, Inflammation, Persistent epithelial defects, Ulceration, Neovascularization, and Conjunctivalisation.
- Diagnosed by – Impression cytology – Goblet cells in the cornea
Middle vascular layer (Uvea)
Consists of 3 things the Iris, Ciliary body and Choroid
Iris – Anterior part of Uvea, Divided by a collarette into Pupillary and ciliary.
Two muscles Sphincter pupillae (Constricts the pupil) and Dilator Pupillae (Dilates the pupil)
Major arterial circle – Present on the root of the iris (Ciliary Body face) – responsible for Hyphema (D-shaped pupil) formation during blunt trauma.
Minor arterial circle – In the collarette between pupillary and ciliary iris.
Ciliary Body – Anterior part – Pars Plicata and Posterior part – Pars Plana
Function – Aqueous Humor production and Accommodation reflex.
Pars Plana – through which only you can enter into Vitreous Humor (to aspirate fluids or for surgery).
The maximum risk of sympathetic ophthalmitis.
Choroid – The most vascular structure of the eye (85% of ocular blood flow)
Vortex veins of the eye are the veins that drain the blood from the uvea particularly the choroid.
Supplies nutrients to the outer retina and is responsible for thermoregulation.
4 layers – Choriocapillaries layer, Bruch’s membrane, and Haller, Sattler.
Malignant Melanoma of Choroid – m/c ocular tumor in adults.
Inner Neural layer (Retina)
Stretches from Fovea to Ora Serrata.
Central retina – Fovea (Brightest and sharpest images formed here), optic disc, and macula.
Peripheral retina – Ora Serrata (thinnest part)
Light passes through the outer retina – Photoreceptors in the outer retina – neural signals – reverse order to the inner retina – optic nerve.
5 types of neurons – Photoreceptors (rods and cones), Bipolar, ganglion, amacrine, and horizontal
3 neuroglial cells – Mullar’s, astroglia, microglia
| Difference Between Rods and Cones | |
|---|---|
| Rods | Cones |
| Peripheral | Central |
| 120 million (20) | 6 million (1) |
| One type | 3 – Red, Blue, and Green |
| Peripheral, Night and Black and white vision | Central, Daylight, and Colour vision |
Anterior Chamber
Between cornea and iris
filled by Aqueous humor
Anterior chamber depth (3mm) – Center of the cornea to the center of the anterior capsule of the lens.
Deep (Young males and Myopes) and shallow chambers (women, elderly and children, Hypermetropes).
The volume of AC – 250 μL
>2.1mm leads to angle-closure glaucoma.
AC angle ( Van Herrick’s method) – Angle between iris and corneal endothelium at the junction of the limbus.
AC structures – Iris, Ciliary Body Band, Scleral Spur, Trabecular meshwork, and Schwalbe’s line.
ACAID (AC Associated Immune Deviation) – Immunologically privileged site.
Crystalline Lens
Biconvex, transparent and avascular structure.
Nucleus, Cortex, and Capsule (Anterior and Posterior).
Water- 65%, Proteins – 35%
90% of lens proteins – crystallins
Function – transmits and focus light on the retina and Accommodation
19D of the 60D of power of the eye.
Nutrition from AH.
Capsule (AC and PC thinnest), Lens epithelial cells (only in the anterior part of the lens), and Lens fibers.
Zonules (Suspensory ligaments) (from Pars Plicata) is holding the lens.
Posterior Chamber is also filled with AH.
Pupil connects AC and PC.
Vitreous Humour
Glassy transparent gel between lens and retina.
4ml volume
99% of water, Hyaluronic acid, and collagen fibers.
Shock absorber, optical media and maintains shape.
Produced at birth.
Attached to disc margin, macula, vitreous base (Ora Serrata), Posterior capsule by Weiger’s ligament.
Access only through Pars Plana.
Aquous Humour
Produced by the non pigmented epithelium of Pars plicata.
Secretion(70%), Ultrafiltration and Diffusion(30%).
Rate of production – 2.50 μL per minute.
Outflow rate – C value – 0.20 μL/ mm Hg/ minute.
IOP – atleast 10 mm Hg.
Composition – Similar to blood but Increased ascorbate and lactate, decreased glucose, a low protein present in AC.
Supplies nutrients to the lens and cornea, removes waste products, macrophages, and blood debris.
AH passage = Pars plicata – PC – Pupil – AC – AC angle – Trabecular meshwork – – Schlemm’s canal – Episcleral veins. (80%)
20% through Uvea Sclearal pathway.
Aquous Humous vs Vitreous Humour
| Aqueous Humour | Vitreous Humour |
| Water | Glass |
| Solution can flow | A gel can’t flow |
| Nutrition | Shock absorber |
| 2.5 μL per minute | At birth |
| Similar to blood | Water, Hyaluronic acid, and Collagen fibers |
| Reached through Limbus | Reached through Pars Plana |
Refractive components
Lens (19D) and Cornea (43D) = + 60D
4 refracting parts (Anterior and Posterior surface of cornea, Anterior and Posterior surface of Lens)
The anterior surface of the Cornea has the most refracting power.
Vasculature of the eye
The principal artery of the eye – Ophthalmic artery – 10 branches.
Most critical one – Central retinal artery – CRA
OA – First branch of ICA
The principal veins of the eye – Central retinal vein/ Vortex veins
Most critical vein – Superior ophthalmic vein
Nerve supply of eye
6 cranial nerves – II, III, IV, V, VI and VII craniel nerves.
ANS – Parasympathetic supply – III cranial nerve – Miosis and accommodation.
Sympathetic supply – V nerve – Mydriasis, Mullar’s muscle (STM), Inferior Tarsal Muscle and sweat glands.
TAKE FREE MCQs on Anatomy of the Eye
I’m Nawin (Admin), a seasoned doctor and accomplished content writer with 8 years of experience. Join me as I unravel the latest breaking news, unveil behind-the-scenes happenings, and explore the aftermath scenes. With my expertise, I’ve crafted this renowned news site to provide you with an authentic perspective on daily happenings. Get ready to delve into a world of truth and knowledge on Medico Topics.
